 
Content framework analysis was applied to the qualitative findings. 
A purposive sample of senior clinicians who ceased resuscitation and applied the checklist were interviewed. Unexpected results which required exploration were identified and developed into semi-structured interview questions. A consecutive sample of checklist data for adult pulseless electrical activity were retrieved from 1st December 2015 to 31st December 2018. Design and methodsĪn explanatory sequential mixed method study was conducted in one ambulance service in the South West of England. This study aimed to describe the patient, clinical and system factors and examine senior clinician experiences when ceasing resuscitation for pulseless electrical activity. To support these decisions, one ambulance service has applied a locally derived cessation of resuscitation checklist. Senior clinicians include paramedics employed to work beyond the scope of clinical guidelines as there may be a point at which it is reasonable to cease resuscitation. Treat the possible causes as you work through H’s and T’s.Evidenced-based guidelines on when to cease resuscitation for pulseless electrical activity are limited and support for paramedics typically defaults to the senior clinician. Once advanced airway is in placed, give 1 breath every 5-6 seconds (10-12 breaths/min) with continuous chest compressions. Consider securing an advanced airway, and capnography. If the rhythm becomes shockable, defibrillate. Establish an IV line and administer Epinephrine every 3-5 minutes. Monitor the ECG and check for a pulse every two minutes. Pulseless Electrical Activity (PEA) Treatment However, in PEA, there is no pulse with an orderly cardiac electrical activity similar to normal sinus, which is not a typical cardiac arrest ECG rhythm like asystole (flatline), ventricular fibrillation or ventricular tachycardia. The absence of a pulse confirms a clinical diagnosis of cardiac arrest. Therefore in PEA, it is important to treat the symptoms of the patient and not merely the rhythm displayed on the monitor. The ECG interpretation can appear the same as a normal sinus rhythm. Pulseless Electrical Activity (PEA) DiagnosisĪn electrocardiogram (ECG/EKG) device is capable of distinguishing PEA from other causes of cardiac arrest. You can also check for heart sounds by using a stethoscope for a period of no more than 10 seconds. Make sure to check for a pulse at the carotid artery. 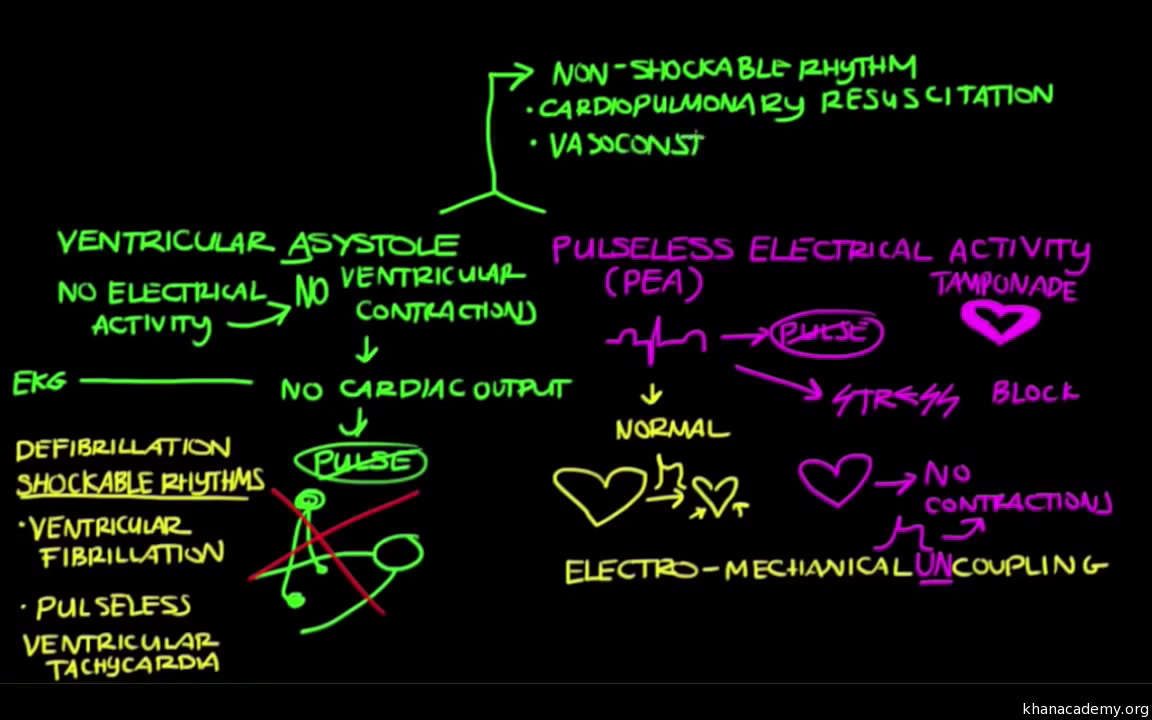
The skin may appear pallor due to no oxygen in the blood. PEA leads to a loss of cardiac output and discontinues blood supply to the brain. Treatable Causes of Pulseless Electrical Activity (PEA)Ī patient with PEA will be unconscious with no breathing and no pulse. An ACLS practitioner should review the Hs and Ts to help identify and treat the cause of the PEA. Possible underlying causes should be identified and treated while CPR is in progress. The electrical activity is dissociated from the mechanical heart function.Ĭardiopulmonary resuscitation (CPR) is the prime treatment for PEA. In PEA, the heart’s electrical activity is present, but the heart muscle is not responding to the electrical impulses. The electrocardiogram (ECG) interpretation displays heart rhythm activity with similarities to a normal sinus rhythm, but the patient has no palpable pulse. Pulseless electrical activity (PEA), is classified as a form of cardiac arrest. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
